
Coccyx pain from running is most commonly caused by weak gluteal muscles, tight pelvic floor muscles, and repetitive impact on hard surfaces. The tailbone absorbs significant shock during each stride, and when the surrounding muscles fail to cushion that impact, the coccyx and its ligaments become irritated and inflamed — sometimes after just a few weeks of increased mileage.
✓ Reviewed by Dr. Sarah Mitchell, Physiotherapist | Last updated: March 2026 | Evidence-based guide

If you've started noticing a deep, nagging ache at the very base of your spine during or after runs, you're not alone. Running-related coccyx pain — clinically known as coccydynia — is an underreported but surprisingly common issue among both recreational joggers and seasoned marathon runners.
The frustrating part? Most runners don't connect tailbone discomfort to their running habit. They assume they bruised something or slept awkwardly. But the biomechanics of running place real, measurable stress on the coccyx, and when certain risk factors converge, pain develops.
This guide explains exactly why running triggers tailbone pain, what's happening anatomically, and — most importantly — the proven strategies to fix it and keep running pain-free.
🩺 Dealing with tailbone pain? Get the complete physio-designed recovery protocol.
Get the 30-Day Protocol — $27 →Your coccyx — the small triangular bone at the very bottom of your spine — is made up of 3 to 5 fused vertebrae. It's far from a useless "vestigial tail." The coccyx serves as an anchor point for the pelvic floor muscles, the gluteus maximus, and several ligaments that stabilise your pelvis during movement.
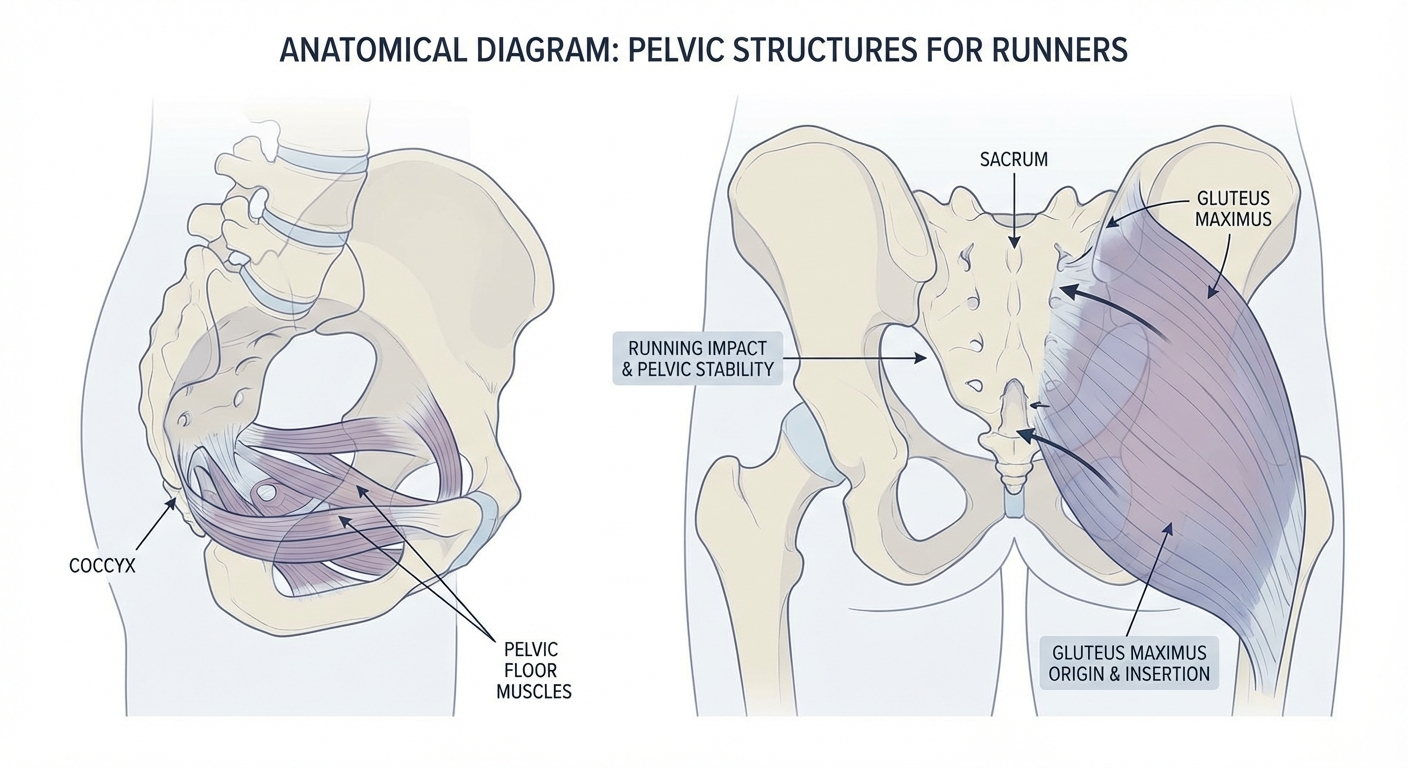
When you run, each foot strike generates ground reaction forces of 2 to 3 times your body weight. These forces travel upward through your legs, pelvis, and sacroiliac joints. The coccyx, sitting at the bottom of this kinetic chain, absorbs a portion of that impact.
In a healthy runner with strong glutes and a well-functioning pelvic floor, the muscular system absorbs most of this shock. The coccyx barely notices. But when muscle imbalances, tightness, or biomechanical issues are present, the coccyx takes on disproportionate stress — and that's when pain begins.
The joint between your sacrum and coccyx (the sacrococcygeal joint) has limited mobility — it flexes slightly when you sit and extends when you stand. Repetitive running impact can inflame this joint, causing a dull ache that worsens with continued activity or prolonged sitting after a run. This joint inflammation is one of the most common diagnoses in runners with tailbone pain.
Understanding the root cause of your running-related tailbone pain is essential for choosing the right fix. Here are the seven most common culprits, ranked by how frequently physiotherapists encounter them:
Your gluteus maximus is the largest muscle in your body and the primary shock absorber during running. It decelerates your leg on each landing and propels you forward during push-off. When the glutes are weak — which is extremely common in people who sit at desks all day — other structures compensate. The hamstrings overwork, the pelvis becomes unstable, and the coccyx absorbs forces it wasn't designed to handle.
Research consistently shows that gluteal weakness is the single biggest biomechanical predictor of running-related lower back and pelvic pain, including coccydynia.
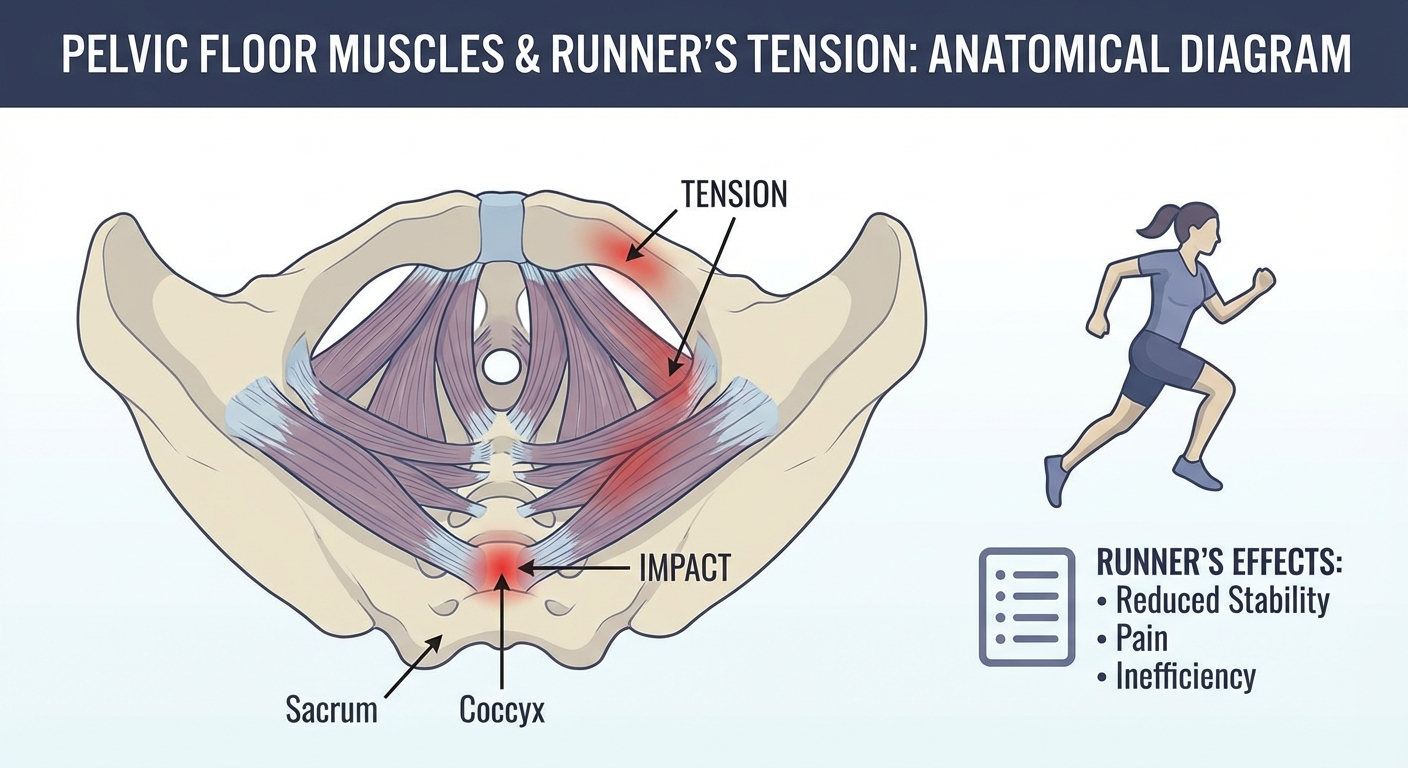
The pelvic floor muscles attach directly to the coccyx. In runners — particularly women and those with high training volumes — these muscles can become hypertonic (chronically tight). A tight pelvic floor pulls on the coccyx with every stride, creating a repetitive strain that leads to inflammation and pain.
This is often missed because pelvic floor issues are associated with post-pregnancy problems, not running. But research shows that high-impact sports like running significantly increase pelvic floor muscle tone, sometimes beyond what's healthy.
Concrete and asphalt are the worst surfaces for coccyx pain. They return nearly 100% of impact force back into your body, compared to grass or trails which absorb 30–50% of impact energy. Runners who train exclusively on roads and footpaths expose their coccyx to significantly higher cumulative loading.
When your foot lands well ahead of your centre of mass (overstriding), braking forces spike dramatically. These braking forces shoot up through the kinetic chain and load the pelvis and coccyx more aggressively than a midfoot or forefoot strike pattern. Overstriding also tends to increase pelvic tilt, which shifts more weight onto the coccyx.
The "too much, too soon" rule applies to coccyx pain just as much as it does to shin splints or IT band syndrome. Increasing weekly mileage by more than 10% per week doesn't give the coccygeal ligaments, sacrococcygeal joint, and pelvic floor muscles time to adapt. Overuse inflammation develops gradually and can take weeks to become noticeable.
If you've ever fallen hard on your tailbone — from a slip on ice, a cycling crash, or a sports accident — the coccyx may have sustained a fracture or dislocation that healed in a suboptimal position. A misaligned coccyx is more vulnerable to running impact because the forces distribute unevenly across the sacrococcygeal joint.
Sitting immediately after a run — especially on a hard chair — is one of the worst things you can do for a sensitive coccyx. Post-run, the pelvic floor and gluteal muscles are fatigued, blood flow to the area is elevated, and the tissues are in a heightened inflammatory state. Sitting compresses the coccyx at exactly the wrong moment.
Not all lower back or buttock pain is coccyx-related. Here's how to distinguish true coccydynia from other running injuries:
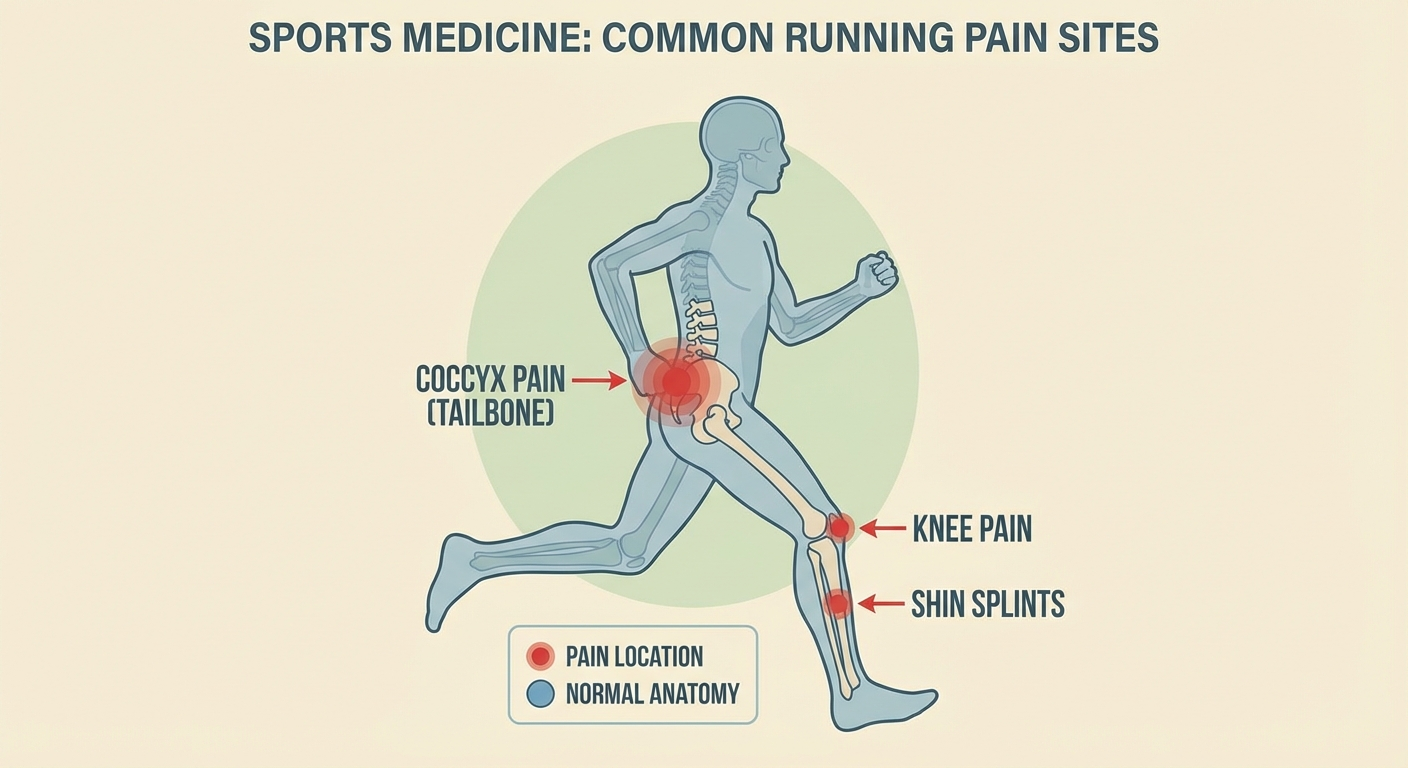
The good news: running-related coccyx pain is highly preventable. Most cases respond to straightforward changes in training, form, and recovery habits. Here are the eight strategies with the strongest evidence behind them.
This is non-negotiable. Add dedicated glute work 2–3 times per week, focusing on gluteus maximus and medius. Bridges, clamshells, single-leg deadlifts, and lateral band walks should be staples. Strong glutes absorb shock, stabilise the pelvis, and take stress off the coccyx. Most running physiotherapists consider this the single most important prevention measure.
Learn diaphragmatic breathing techniques that help relax the pelvic floor. Deep belly breathing with a slow exhale directly counteracts pelvic floor hypertonicity. Consider seeing a pelvic floor physiotherapist if you suspect chronic tightness. Child's pose and deep squat holds also help release these muscles.
Never increase weekly running volume by more than 10%. This gives the sacrococcygeal ligaments and pelvic floor adequate time to adapt. If you're returning from a break, start at 50% of your previous volume and build back gradually over 4–6 weeks.
Alternate between soft surfaces (grass, trails, track) and hard surfaces (road, footpath). Aim for at least 40% of your weekly mileage on softer surfaces. If you're currently symptomatic, shift temporarily to 100% soft surfaces until pain resolves.
A higher running cadence (steps per minute) naturally shortens your stride and reduces overstriding. Most recreational runners benefit from increasing cadence by 5–10%. Use a running app or metronome — aim for 170–180 steps per minute. This single change reduces peak impact force by up to 20%.
Walk for 10–15 minutes after finishing your run before sitting down. When you do sit, use a coccyx cushion to reduce direct pressure on the tailbone. This simple habit prevents post-run inflammation from being aggravated by compression.
Tight piriformis and hip flexor muscles alter pelvic mechanics and increase coccygeal loading. Spend 5 minutes daily on figure-four stretches, pigeon pose, and kneeling hip flexor stretches. Hold each stretch for 30–60 seconds, never bounce.
Worn-out running shoes lose their shock absorption capacity after 400–500 miles. If your shoes are past this point, they're transmitting significantly more impact to your pelvis and coccyx. Replace them on schedule, and consider shoes with enhanced cushioning if you run primarily on hard surfaces.
🩺 Need a structured recovery plan? Our 30-day protocol includes all the exercises above — with daily progressions.
Get the 30-Day Protocol — $27 →These five exercises target the exact muscle groups that protect the coccyx during running. Perform them 3 times per week on non-running days, or as a warm-up before easy runs. For a complete daily schedule with progression guidelines, our 30-Day Coccyx Relief Protocol lays out the full program.

Lie on your back, knees bent, feet flat. Drive through your heels and squeeze your glutes to lift your hips. Hold the top position for 2 seconds. Lower slowly. This targets gluteus maximus — the primary shock absorber for the coccyx. Progress to single-leg bridges once you can do 3 × 15 comfortably.
Lie on your side, knees bent at 45 degrees, feet together. Keeping feet touching, open your top knee like a clamshell. Hold 1 second at the top. This strengthens gluteus medius, which stabilises the pelvis during the single-leg stance phase of running. Add a resistance band above the knees to progress.
Kneel and sit back on your heels, arms extended forward, forehead on the floor. Breathe deeply into your belly — inhale 4 seconds, exhale 6 seconds. This gently stretches the pelvic floor and lower back while promoting parasympathetic relaxation. Especially useful post-run.
Lie on your back. Cross one ankle over the opposite knee. Pull the bottom knee toward your chest until you feel a deep stretch in the crossed-leg buttock. The piriformis sits directly over the coccyx region — releasing it reduces compression on the tailbone.
Start on all fours. Extend your right arm and left leg simultaneously, hold 2 seconds, return. Switch sides. This trains core stability and coordinated glute activation — both essential for reducing pelvic instability that contributes to coccyx pain during running.
Small changes to your running mechanics can dramatically reduce the forces reaching your tailbone. Focus on these three adjustments:
Research published in Medicine & Science in Sports & Exercise found that increasing running cadence by just 5–10% reduces vertical impact loading rate by 15–20%. A higher cadence means shorter strides, which means your foot lands closer to your centre of mass, reducing braking forces and coccygeal loading.
How to do it: Check your current cadence with a running watch or phone app. If you're below 170 steps per minute, gradually increase by 5% every 2 weeks. Use a metronome app set to your target cadence during easy runs.
A subtle forward lean (2–3 degrees from vertical) shifts your foot strike point back under your body and reduces posterior pelvic loading. Think of "falling forward" rather than reaching out with your legs. This naturally encourages a midfoot strike and reduces the braking forces that load the coccyx.
Many runners develop an anterior pelvic tilt (arched lower back) or posterior tilt (tucked pelvis) when fatigued. Both positions increase coccygeal stress. Imagine your pelvis is a bowl of water — keep it level. Strong core muscles maintain this neutral position longer into a run.

Your shoes and the ground beneath them are your first line of defence against impact forces reaching the coccyx.
If you're currently experiencing coccyx pain, consider temporarily switching all your runs to soft surfaces. Many runners find their symptoms resolve within 2–3 weeks just by making this change — without reducing mileage at all.
If you're currently dealing with running-related coccyx pain, here's a phased return-to-running protocol based on physiotherapy best practices:
🩺 Our 30-Day Coccyx Relief Protocol follows exactly this phased approach — with daily exercises, checklists, and progression criteria.
Get the Full Protocol — $27 →Most running-related coccyx pain resolves with the self-management strategies above. However, you should seek professional evaluation if:
A physiotherapist specialising in pelvic health or sports medicine can perform a thorough assessment including pelvic floor muscle tone testing, gluteal strength assessment, and running gait analysis. Imaging (X-ray or MRI) is usually only needed if a fracture, dislocation, or other structural pathology is suspected.
For general tailbone pain management beyond running, our comprehensive guide to tailbone pain relief covers cushioning strategies, targeted exercises, sleep positions, and more.
Tailbone pain after running is typically caused by repetitive impact forces transmitted through the pelvis, tight pelvic floor muscles, weak gluteal muscles that fail to absorb shock, or poor running form that increases coccygeal loading. In rare cases, a stress reaction in the coccyx itself can develop from overtraining.
Running rarely causes direct coccyx fracture, but repetitive impact can cause coccygeal bruising, inflammation of the sacrococcygeal joint, or stress reactions in the tailbone. Falls during trail running are a more common cause of acute coccyx injuries in runners.
You don't necessarily need to stop completely. Reduce your mileage by 50%, switch to softer surfaces like grass or trails, and incorporate the stretching and strengthening exercises recommended for coccyx pain. If pain persists beyond 2 weeks despite modifications, see a physiotherapist or doctor.
Softer surfaces like grass, dirt trails, and rubberised athletic tracks reduce impact forces by 30–50% compared to concrete or asphalt. Treadmills with cushioned decks are also a good option. Avoid concrete sidewalks, which transmit the highest impact forces to the pelvis and tailbone.
Yes. Weak gluteus maximus and medius muscles are a leading biomechanical cause of running-related coccyx pain. The glutes act as primary shock absorbers during the landing phase of running. When they're weak, more impact force is transferred to the pelvis and coccyx, causing pain and inflammation.
Most running-related coccyx pain resolves within 4 to 8 weeks with proper management including activity modification, targeted stretching, glute strengthening, and surface changes. Chronic cases involving sacrococcygeal joint inflammation may take 3 to 6 months with physiotherapy guidance.
This article is based on peer-reviewed research, clinical guidelines, and physiotherapy best practices. All claims are referenced below. Content has been reviewed by a qualified physiotherapist.
🩺 Ready to fix your tailbone pain? Get the complete physio-designed 30-day recovery protocol.
Get the 30-Day Protocol — $27 →